Chronic Fatigue Treatment Center in Chapel Hill
If you struggle with Chronic Fatigue, our certified Neurofeedback doctors at Leigh Brain & Spine can perform the proper testing needed in order to create a treatment plan for a more comfortable and better way of life.
What is Chronic Fatigue Syndrome?
Chronic Fatigue Syndrome is a complicated disorder with neurological bases. Science shows that it has a brain pattern at the root of its cause. It is characterized by extreme fatigue that gets worse with exertion of your mind or body, however, the fatigue can’t be explained by other underlying medical conditions. The fatigue does not get better after rest. People with Chronic Fatigue Syndrome feel tired all the time and cannot get over it through the usual means.
Causes
What Causes Chronic Fatigue Syndrome?
The medical term for Chronic Fatigue Syndrome is Myalgic Encephalomyelitis (ME). When we dissect this term we come to understand that it means “muscle pain or tenderness” (myalgic) from “inflammation of the brain and spinal cord” (encephalomyelitis).
What Are the Risk Factors for Chronic Fatigue?
Factors that may increase your risk of chronic fatigue syndrome include:
- Age. Chronic fatigue syndrome most commonly occurs in people between 40 and 60 years of age.
- Sex. Women suffer from Chronic Fatigue Syndrome at a striking rate compared to men. This might be because more women are reporting their symptoms or women are at a greater risk for the brain pattern that is associated with CFS.
- Infection & Low Immunity. Viral infections have been associated with the onset of CFS as a by-product of a low immune response.
- Stress. Difficulty managing stress may contribute to the development of chronic fatigue syndrome.
Underlying Factors that Might Cause or Contribute to Chronic Fatigue Syndrome
Hypersensitivity to typical amounts of physical or mental activity due to lower overall brain activation as identified on qEEG neurometric assessments. Triggers might include:
- Viral infections might make symptoms worse.
- Immune system problems can contribute lower brain activation and increased inflammation.
- Stress
Symptoms
What Symptoms are Associated with Chronic Fatigue Syndrome?
A core set of symptoms that affect nearly everyone with CFS exists. The symptoms may come on suddenly for some and may come gradually over days or weeks for others. For some people the symptoms wax and wane, becoming better and worse, over time. For others, the symptoms stay consistent and debilitating. Signs and symptoms may include:
- Fatigue
- Memory Loss or Concentration Difficulties
- Muscle or Joint Pain
- Headaches
- Sore Throat
- Enlarged Lymph Nodes
- Sleep that is non-restorative and doesn’t feel refreshing
- Extreme exhaustion lasting more than 24 hours after physical or mental exercise
What Complications Might Occur Because of Chronic Fatigue Syndrome?
People with Chronic Fatigue have been shown to have a greater risk of:
- Depression
- Stress
- Social Isolation due to restricting their activities
- Not being able to work
How Can You Reduce Chronic Fatigue Symptoms Fast?
Although there is no cure for Chronic Fatigue Syndrome it is known that it is caused and made worse by three factors: (1) the brain pattern associated with Chronic Fatigue Syndrome, (2) Stress, which is correlated with another, separate, brain pattern, and (3) Inflammation. When these three factors are addressed in concert, symptoms can reduce and be resolved much more quickly than if they are not. At Leigh Brain & Spine, the doctors identify the disruptive neurological patterns using qEEG Brain Mapping and then regulate those patterns toward optimal functioning using Neurofeedback Therapy. To address inflammation, they perform Food Sensitivity Testing to identify foods that are causing inflammation within the nervous symptom. Foods that your system are sensitive to can be causing symptoms of Chronic Fatigue Syndrome or making them worse.
What are the Biggest Complaints of People With Chronic Fatigue Syndrome?
Extreme physical or mental fatigue, or both can be experienced by those with CFS. The fatigue can be constant, or it can come and go, and it is not relieved by rest. Usually the fatigue is so severe that it interferes with your ability to work, to engage in recreational and social activities. Sleep can be seriously disrupted due to CFS and pain can be constant. Chronic Fatigue can also cause problems with concentration, memory, or being able to hold your own in a conversation. Confusion, slow thinking and disorientation can happen also and might be accompanied by physical symptoms muscle weakness or muscle coordination difficulties. Having depression along with CFS is common and can make symptoms worse. Science proves that those with Chronic Fatigue Syndrome suffer widely from depression but not vice versa. CFS causes symptoms that are the same as many other diseases, especially early on. For this reason, CFS can be diagnosed only after a thorough evaluation has ruled out other conditions with similar symptoms. The brain pattern associated with CFS can be confirmed using qEEG and brain-based therapies can be identified as a possible solution.
Therapies
How Can Brain-based Therapies Help Chronic Fatigue Syndrome?
What’s the Best Test to Identify Chronic Fatigue Syndrome?
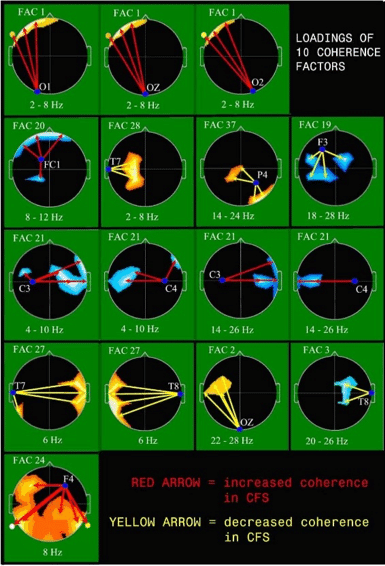 Chronic Fatigue has been shown to be correlated with a specific brain functioning pattern that creates the symptoms associated with the disorder. A recent study from Stanford University shows EEG correlates of Chronic Fatigue Syndrome in the brain demonstrating lower overall brain activation that causes the feelings of fatigue on an ongoing basis. Another study from Harvard University showed significant differences in communication between brain areas, known as coherence. Dr. Frank Duffy of Harvard Medical School commented, “This fundamental finding indicates that CFS patients manifest patterns of functional brain coupling that differ from those of normal controls. Such a difference of CFS brain physiology may help explain known differences in cognition, memory, sleep, and affect that afflict CFS patients.” Dr. Duffy concluded the article by stating that the identification of this brain pattern through qEEG testing may be a key to helping patients with Chronic Fatigue Syndrome.
Chronic Fatigue has been shown to be correlated with a specific brain functioning pattern that creates the symptoms associated with the disorder. A recent study from Stanford University shows EEG correlates of Chronic Fatigue Syndrome in the brain demonstrating lower overall brain activation that causes the feelings of fatigue on an ongoing basis. Another study from Harvard University showed significant differences in communication between brain areas, known as coherence. Dr. Frank Duffy of Harvard Medical School commented, “This fundamental finding indicates that CFS patients manifest patterns of functional brain coupling that differ from those of normal controls. Such a difference of CFS brain physiology may help explain known differences in cognition, memory, sleep, and affect that afflict CFS patients.” Dr. Duffy concluded the article by stating that the identification of this brain pattern through qEEG testing may be a key to helping patients with Chronic Fatigue Syndrome.How Can Brain-based Therapies Help Chronic Fatigue Syndrome?
What’s the Most Effective Treatment for Chronic Fatigue?
Since Chronic Fatigue Syndrome does not have a known cure, there is no one treatment that has been proven to work best for all people. A qEEG Brain Map would show you if you have the brain pattern that is associated with Chronic Fatigue Syndrome and if the pattern of Stress might be making symptoms worse as well. Neurofeedback Therapy can then change the brain pattern toward a more optimal one proven to be symptom-free. When the brain is using a better neurological pattern, the flow of information from the brain to the body through the spinal nerves, is improved and symptoms can be reduced. Food Sensitivity Testing and Gut Repair can have powerful anti-inflammatory effects and can reduce the swelling to help the brain and nerves function better. Also, physiological therapies can help to stimulate the nerves, preventing long-term symptoms to persist. This is a comprehensive neurological approach proven to have maximal impact on improving symptoms for those who suffer with Chronic Fatigue Syndrome.
What Can I Do At Home To Improve My Chronic Fatigue Symptoms?
Do-It-Yourself strategies can be a very important part of decreasing the symptoms associated with Chronic Fatigue Syndrome. Remembering that the CFS brain pattern is shown to be one of less overall activation, it is important to create a schedule to maximize your opportunities when your brain feels more activated and let it recover when it does not. This can help to move your brain pattern in the right direction while controlling your symptoms and giving yourself some relief.
Publications
- EEG Characteristics of Chronic Fatigue Syndrome
- EEG distinguishes Chronic Fatigue from healthy and depressed people


